Delhi Address:
36-A, Pocket 2, Sector 6, Behind Sector 6 Market, Dwarka, Delhi
Gurugram Address:
R2 136 M3M 65th Avenue Sector 65, Golf course extension road. Gurgaon Haryana 122101
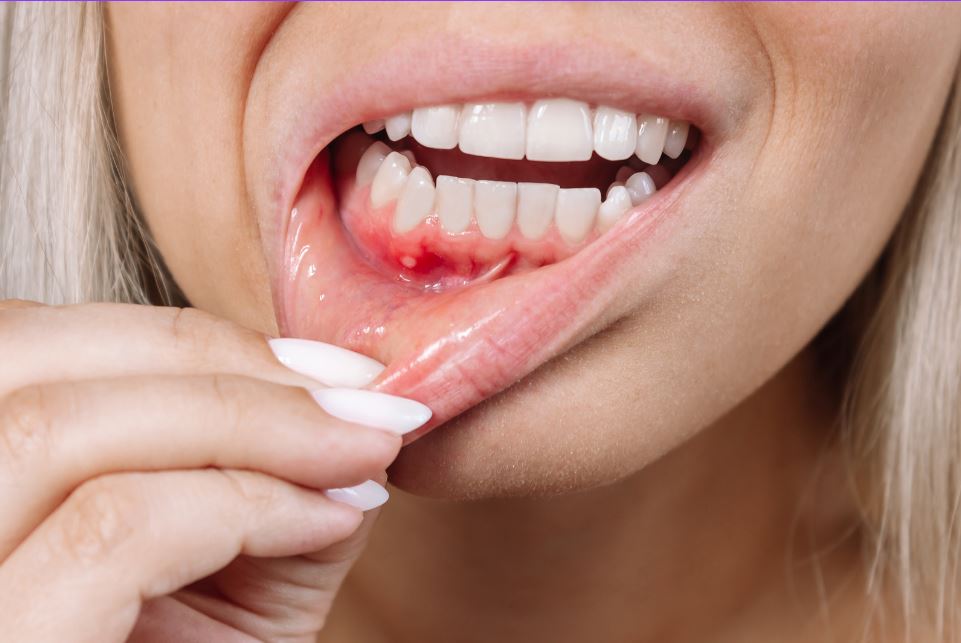
Periodontitis is a common and serious gum disease that affects millions of people around the world. It is a form of periodontal disease that primarily affects the tissues surrounding and supporting the teeth, including the gums, ligaments, and bone. If left untreated, it can lead to tooth loss and other severe health complications.
The primary cause of periodontitis is bacterial plaque buildup on the teeth and along the gum line. Plaque is a sticky film made up of bacteria, mucus, and food particles that constantly form on our teeth. When plaque is not removed through proper oral hygiene practices such as brushing and flossing, it hardens into tartar (calculus), which can only be removed by a professional dental cleaning.
As tartar builds up along the gum line, it creates a space or pocket between the gums and teeth where more bacteria can thrive. This leads to inflammation of the gums (gingivitis) which causes them to become red, swollen, and bleed easily. If gingivitis is not treated promptly, it can progress to periodontitis.
The early stages of periodontitis may not have noticeable symptoms, which is why regular dental checkups are crucial. However, as the disease progresses, some common signs and symptoms may include persistent bad breath, swollen or receding gums, loose teeth, and changes in the way your teeth fit together when you bite.
If you experience any of these symptoms, it is important to seek treatment from a periodontist as soon as possible. The first line of treatment for periodontitis is a deep cleaning procedure called scaling and root planning that removes plaque and tartar from above and below the gum line. In more severe cases, surgical procedures may be necessary to restore damaged tissue or bone.
Periodontitis, also known as pyria, is a serious oral health condition that affects the tissues and bones supporting your teeth. Some of the common causes of periodontitis are listed below:
The most common cause of periodontitis is poor oral hygiene. When plaque and bacteria are not removed regularly from the teeth and gums through brushing and flossing, they can build up and cause inflammation in the gums. This eventually leads to gum disease if left unaddressed.
Smoking or using other forms of tobacco has been linked to an increased risk of developing periodontal disease. Tobacco use weakens the immune system, making it harder for your body to fight off infections in your gums.
Some individuals may be genetically predisposed to developing periodontitis due to inherited traits from their parents or family members with a history of gum disease.
People with diabetes are more prone to developing periodontal disease due to their weakened immune system and difficulty in controlling blood sugar levels. High blood sugar levels can also make it easier for bacteria to thrive in the mouth, increasing the risk of gum infections.
Hormonal changes during pregnancy or menopause can increase sensitivity in the gums, making them more susceptible to infections and leading to periodontal disease.
Certain medications like anticonvulsants, immunosuppressants, and calcium channel blockers have been linked to an increased risk of gum disease as they can reduce saliva production or cause abnormal growth of gum tissue.
Breathing through your mouth instead of your nose can dry out your mouth's protective saliva layer, leaving you more vulnerable to plaque buildup on teeth and leading to periodontal disease.
A diet lacking in essential nutrients can weaken the immune system, making it difficult for your body to fight off infections and increasing the chances of developing periodontitis.
Persistent bad breath or a bad taste in your mouth can be an indicator of periodontal disease. The foul odour results from bacterial build-up in deep pockets around teeth as well as decaying tissue due to a lack of proper dental hygiene.
As periodontal disease progresses, it causes the gums to pull away from the teeth, creating gaps called pockets between them. These pockets filled with bacteria cause further infection and destruction of bone and connective tissue that hold teeth in place.
Gum recession exposes more sensitive parts of your tooth such as roots which are not covered by enamel leading to sensitivity when eating hot/cold foods.
Advanced stages of periodontal disease result in loosening teeth due to destruction occurring in supporting structures like bones causing them to shift position when you bite down.
As teeth loosen up and move out of alignment due to advanced gum disease they may alter how upper/lower ones come together resulting in a noticeable change.
Chewing food becomes uncomfortable if you have periodontitis because infected gums are sensitive even if it doesn't come in contact with food. As the disease worsens, chewing may also cause pain due to loose teeth.
Periodontitis can also cause pus formation in areas around teeth resulting from infection. It may appear as a white or yellow substance that oozes from the gums and is accompanied by a foul odour and taste.
The first step in diagnosing periodontitis is a thorough physical examination of the mouth by a periodontist. The periodontist will check for signs of inflammation, swelling, redness, bleeding, and recession of the gums. They will also measure the depth of any pockets between the teeth and gums using a small ruler called a probe. This helps determine the severity of the disease.
Dental X-rays are commonly used to diagnose periodontal disease as they allow dentists to see what’s happening beneath the gum line. These images help identify any bone loss that may have occurred due to advanced periodontitis.
Periodontal disease is caused by an overgrowth of harmful bacteria in the mouth. To confirm this, a bacterial test may be performed to identify specific bacteria present in plaque or tartar buildup on teeth and root surfaces.
During this process, Periodontist will use a special tool called a probe to measure pocket depths around each tooth while recording them on a chart known as a “periodontal chart”. This provides valuable information about any changes occurring over time and allows for better tracking of treatment progress.
Periodontitis can cause significant discomfort and pain for some individuals depending on its severity level; therefore, your periodontist needs to assess and document any pain or sensitivity you may be experiencing in the affected area.
Early diagnosis of periodontitis is crucial for effective treatment and prevention of further damage.
Periodontitis is a serious gum disease that can lead to tooth loss if left untreated. Fortunately, there are various treatment options available to help manage and improve the condition. The type of treatment recommended will depend on the severity of the periodontitis and other factors such as overall health and medical history.
The main goal of treating periodontitis is to control the infection and prevent further damage to the gums, teeth, and supporting bone structures.
Here are some common treatment options for periodontitis:
It is essential to note that periodontitis is a chronic disease, meaning it cannot be cured but can be managed with proper treatment. It is crucial to follow your periodontist's recommended treatment plan and attend regular check-ups and cleanings to prevent the disease from progressing.
Pyria is a serious infection that affects the tissues surrounding and supporting the teeth. If left untreated, it can lead to severe damage to the gums and even tooth loss. However, there are steps you can take to prevent and manage periodontitis.
Despite being a common oral health issue, there are still many myths and misconceptions surrounding periodontitis. These false beliefs can lead to misunderstandings about the condition, its causes, symptoms, and treatment options. Here we are mentioning some of the most prevalent myths along with evidence-based information to help you better understand periodontitis.
One of the most common misconceptions about periodontitis is that it only affects individuals with poor oral hygiene habits. While it is true that inadequate brushing and flossing can increase your risk of developing gum disease, there are other factors at play as well. Genetics, certain medications, hormonal changes in women, smoking, and underlying health conditions like diabetes can all contribute to the development of periodontitis. Therefore, even if you have excellent oral hygiene habits, you may still be susceptible to this condition.
Many people believe that bleeding gums during brushing or flossing are normal and nothing to worry about. However, this is not true. Bleeding gums are often an early sign of gum disease and should not be ignored. If left untreated, it can progress into periodontitis and cause more severe symptoms such as receding gums and tooth loss.
While some risk factors for periodontitis cannot be controlled (such as genetics), there are steps you can take to prevent its development or slow its progression if you already have it.
Another common myth is that gum disease only affects the mouth. In reality, periodontitis has been linked to several systemic health issues such as heart disease, stroke, respiratory problems, and complications during pregnancy. The bacteria from infected gums can enter the bloodstream and travel to other parts of the body, causing inflammation and potentially leading to serious health problems.
Fortunately, there are many treatment options available for periodontitis. Depending on the severity of your condition, your Periodontist may recommend a deep cleaning procedure called scaling and root planning or more advanced treatments like laser therapy or surgery. With proper treatment and good oral hygiene habits at home, you can effectively manage periodontitis and prevent further damage to your gums and teeth.
It is essential to educate ourselves about periodontitis to dispel any myths or misconceptions we may have heard. By understanding its causes, symptoms, and treatment options correctly, we can take proactive steps toward preventing this common oral health issue and maintaining overall health.

